Image: ShutterStock
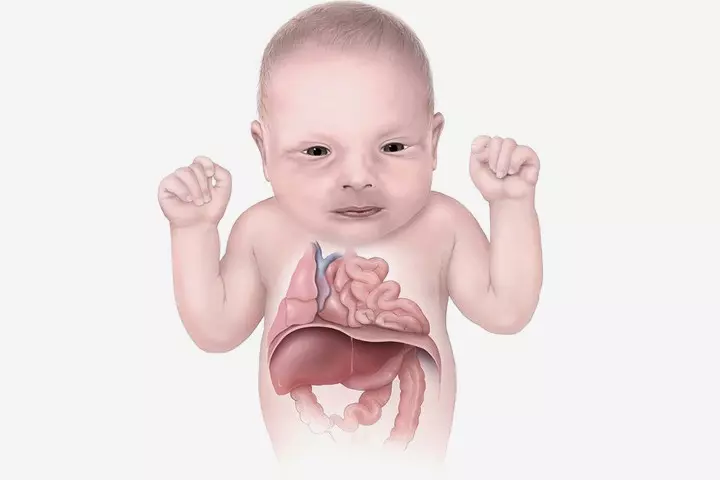
Congenital diaphragmatic hernia in babies or CDH in babies occurs when the diaphragm fails to close during fetal life. The diaphragm is a muscular wall separating the chest and abdominal cavity. If there is an opening, the abdominal organs may herniate or protrude to the chest cavity and affect lung growth.
Babies with CDH may develop pulmonary hypoplasia (resulting in a smaller lung) and pulmonary hypertension (high blood pressure in the lung arteries). Prompt medical care soon after birth may reduce the complications of CDH in babies. However, such babies have an increased risk for morbidity and mortality.
Read on to know about the causes, symptoms, types, complications, diagnosis, and treatment of CDH in babies.
Key Pointers
- Faulty closure of the diaphragm in a fetus causes congenital diaphragmatic hernia or CDH in babies.
- Posterolateral Bochdalek hernia and anterior (Morgagni) hernia are the two types of CDH.
- Neonates with CDH may have complications such as chronic lung diseases, increased lung pressure, or developmental delays.
- Fetal surgery may be considered if severe CDH is detected in ultrasounds.
Causes Of CDH In Babies

Image: Shutterstock
The cause of CDH is unknown in many babies. It is believed to be multifactorial. Some research suggests that genetic factors may cause CDH, especially when it occurs with other birth defects, such as congenital heart defects. However, CDH may also be an isolated anomaly in some babies with no other genetic defects (1).
Source: Centers for Disease Control and Prevention, National Center on Birth Defects and Developmental Disabilities
 Quick fact
Quick factTypes Of CDH
CDH can be of two types (2).
- Posterolateral Bochdalek hernia is the common type (70-75%), occurring due to a hole in the diaphragm’s back. Majority occur on the left side.
- Anterior (Morgagni) hernia (23-28%) occurs due to a hole in the front of the diaphragm. This type of hernia has less impact on lung growth.
- Central (2-7%)
 Experts say
Experts saySigns And Symptoms Of CDH
The following signs and symptoms are seen before birth on the prenatal ultrasound.
- Fluid in the chest
- Displaced heart
- Herniation of liver, intestines, and stomach to the chest cavity
Bochdalek hernia usually causes more severe symptoms (3).
- Fast breathing (tachypnea) or breathing difficulties
- Increased heart rate (tachycardia)
- Bluish skin or cyanosis
- Barrel-shaped chest or chest with abnormal shape, such as one side may look more extensive than the other
- Caved in or scaphoid appearance of the abdomen
- Symptoms of respiratory distress such as grunting respiration and chest retractions
- Other congenital anomalies including cardiac, vertebral, ear etc.
Some babies with CDH may require aggressive resuscitation due to underdeveloped lungs and circulatory insufficiency.
Respiratory distress and cyanosis immediately or a few minutes or hours after birth can be commonly seen in babies with CDH.
Prognosis
All of the following factors are associated with increased risk of mortality and morbidity:
- Presence of associated anomalies, especially those of heart
- Extensive underdevelopment of lungs or lung hypoplasia
- Liver entering chest cavity
Complications Of CDH
After the immediate neonatal period CDH could be associated with the following complications (2).
- Hernia recurrence
- Failure to thrive
- Inability to feed, requiring feeding through tubes
- Chronic lung diseases requiring oxygen therapy such as oxygen supplementation and medications for a long time
- Pulmonary hypertension
- Repeated lung infections
- Developmental delay

Image: Shutterstock
- Gastroesophageal reflux (abnormal positioning of the stomach)
- Hearing impairment
- Chest wall deformities such as scoliosis and pectusiA condition where breastbones grow inwards, causing a mild or severe depression of the chest wall
Complications may vary based on the severity of the CDH. Early interventions are required to minimize the effect of these complications and reduce the risks of any long-term complications.
Diagnosis Of CDH
CDH is diagnosed during prenatal ultrasound since the abdominal organs, such as the stomach, liver, and intestine, may be seen in the chest cavity.
These abdominal organs may push the heart to one side.
The following imaging techniques are often ordered to confirm the prenatal diagnosis of CDH (1).
- High-resolution fetal ultrasound to evaluate the fetal anatomy and CDH
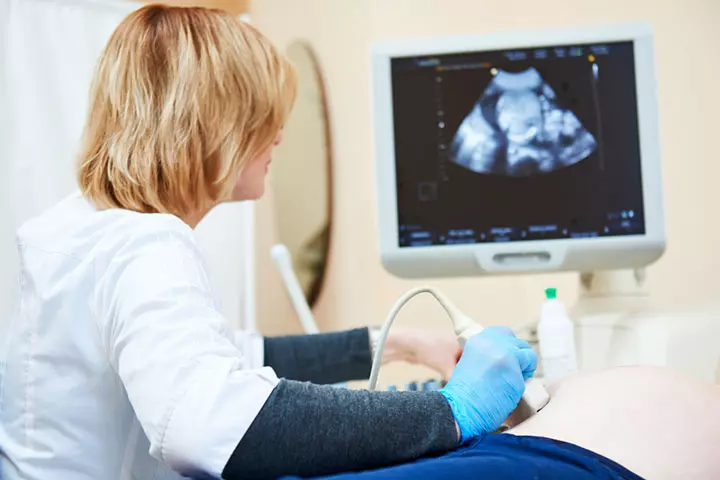
Image: Shutterstock
- Fetal echocardiogramiUse of sound waves to examine baby’s heart issues before birth to assess structure and functions of the fetal heart
- Ultrafast fetal MRI also helps to visualize the anatomy and CDH
These tests identify the affected part of the diaphragm and the displaced organs. CDH may affect the left, right, or both sides of the diaphragm. The impact of CDH on the lungs is also noted to estimate the consequences after birth.
Arundhati Sharma, a mother, recalls her experience when an ultrasound at 24 weeks of gestation showed a possibility of the fetus having CDH. She says, “The radiologist told me the baby is suffering from CDH (Congenital Diaphragmatic Hernia), she further explained that the intestine is pushing our baby’s heart over the right side of its chest, which may hinder his lung growth. After a few minutes, she called in a doctor to study the ultrasound, who then ordered a series of additional tests.” A fetal MRI confirmed the doctor’s suspicion (i).
Treatment Of CDH
Treatment options may vary depending on the severity of CDH and the age of the baby. The treatment can be prenatal or postnatal (4).
1. Management during pregnancy
You may receive a referral to a maternal-fetal medicine specialist and a pediatric surgeon if the prenatal ultrasound shows signs of CDH. The obstetric team managing CDH pregnancies may observe the CDH pregnancies every four weeks until the last trimester and every week after that.
Lung dimensions and amniotic fluid volume measurements on ultrasound are done at frequent intervals during the prenatal period. If the CDH is severe, fetal surgery is considered. Fetoscopic endoluminal tracheal occlusion (FETO) is a fetal surgery for CDH. Treatment before birth could help the baby’s lungs grow correctly and avoid life-threatening complications.
2. Delivery of babies with CDH
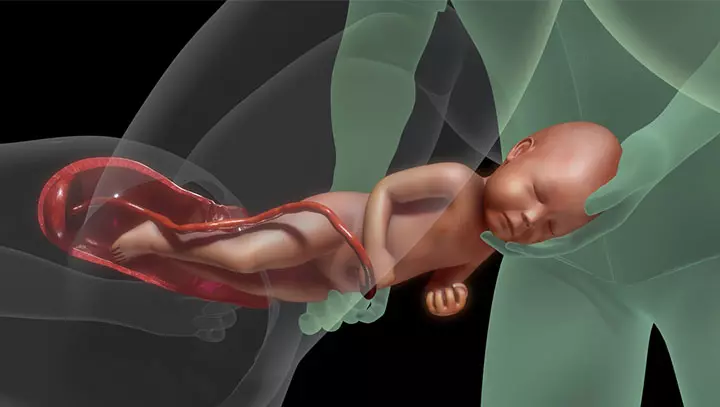
Image: Shutterstock
If the CDH is diagnosed during the prenatal period, delivery is planned in a multispecialty hospital since the baby may require medical care immediately after birth. Most babies with CDH are delivered vaginally at term if there are no obstetric issues necessitating cesarean section.
Many newborns with CDH are transferred to neonatal intensive care units for postnatal care. Breathing tubes and a ventilator (breathing machine) are connected to babies with respiratory distress. A nasogastric or orogastric tubeiSoft tubes inserted through the nose or the mouth into the stomach to provide food or medication is also inserted to keep the stomach decompressed since this may help the lungs expand. Many babies require extensive NICU care for many days.
3. Surgical repair of CDH
Surgical repair of CDH is done through an incision below the rib cage. The time and type of surgery may vary based on the severity and health status of the baby. Medications and inhalation therapies are also given before surgery to enhance lung function. It should be understood that though surgery is a part of long term management it seldom produces acute relief of symptoms.
A Gore-Tex patch or a muscle flap is used to close the diaphragmatic opening, depending on its size. Regular follow-up is done for a few years to observe lung growth in babies.
4. NICU stay for babies with CDH
Babies are kept in NICU since these facilities are immediately available for stabilization. Nitric oxide, high-frequency oscillatory ventilation (HFOV), and ECMO (heart-lung machine) may be required for CDH management.
HFOV can deliver air and pressure against pulmonary hypertension as compared to standard ventilators. ECMO machines take over the functions of the heart and lungs in the body. This provides rest to the lungs and avoids complications due to inadequate lung and heart functions in babies.
The length of hospital stay and outcomes may vary based on the severity of CDH. These babies require follow-up care.
Sharing how the baby’s condition was managed in the hospital after her son was born, Sharma says, “The very next day, his CDH surgery was performed. I was allowed to see him immediately after his surgery… He was kept in an isolated ward so that he didn’t catch any infection, which could result in slow recovery and septic on the stitches. He spent the next two weeks in the NICU.” The child survived the surgery and recovered well.
Frequently Asked Questions
1. Is it possible to breastfeed a baby with CDH?
Some babies with less severe CDH can be breastfed without any complications. Besides severity, clinical conditions and associated anomalies also play a role in determining the possibility of being able to breastfeed.
2. How long do babies with CDH live?
The life expectancy of a baby with CDH may vary depending on the hernia’s type and severity. If the babies survive the acute phase those with severe lung dysplasiaiChronic lung disease usually affecting preterm babies whose lungs are not developed properly may have reduced life expectancy. Many can catch up with the lung growth after repair since the lung may grow until eight years of age. Timely treatment, regular follow-ups, and special therapies may help to achieve normal life expectancy after CDH repair.
3. Can CDH be misdiagnosed?
CDH could be misdiagnosed in some babies since the signs and symptoms are not specific for this condition. This may often occur if there is a late presentation of signs and symptoms. CDH could be often misdiagnosed as pneumonia, pneumothorax, pulmonary effusion, and congenital pulmonary anomalies in some babies. Congenital diaphragmatic hernia (CDH) occurs at birth but many times can be diagnosed prenatally through ultrasound. The postnatal treatment and management depends on the severity of the condition and the presence of other anomalies. Timely treatment could improve outcomes, and the baby could have normal long-term lung and heart functions.
4. Can CDH babies live a normal life?
The long-term effects of CDH depend on the severity of the condition. Children with mild CDH may lead normal, active lives without complications (5).
5. How common is CDH in babies?
CDH is a type of hernia in babies that may be present in about one in 2,200 live births. The condition is usually detected during a prenatal ultrasound in the first or second trimester (5).
6. What is the survival rate of CDH babies?
Congenital Diaphragmatic Hernia in Babies may sometimes lead to complications. It is diagnosed before birth through ultrasound and other imaging modalities. The doctor may carry out this treatment before or after birth based on the severity of the condition and other morbidities. Although CDH in babies is concerning, early diagnosis can help with the timely treatment of the baby. With prompt treatment and necessary preventive measures, there is hope for a positive outcome with a healthy functioning heart and lungs.
Infographic: How To Identify Congenital Diaphragmatic Hernia (CDH)?
CDH affects the development of the diaphragm in babies, leading to various complications. Therefore, knowing the early signs is crucial for timely intervention. The following infographic provides lists of potential signs and symptoms that can be detected in prenatal ultrasounds and in newborns.
Some thing wrong with infographic shortcode. please verify shortcode syntaxCongenital Diaphragmatic Hernia is a birth abnormality in which the diaphragm is affected, causing abdominal organs to be displaced into the chest cavity. Learn more in this video!
Personal Experience: Source
MomJunction articles include first-hand experiences to provide you with better insights through real-life narratives. Here are the sources of personal accounts referenced in this article.
i. Fear of losing;https://mrs-arusharma.medium.com/fear-of-loosing-123990b500c0
References
1. Congenital Diaphragmatic Hernia; Johns Hopkins Medicine
2. Congenital Diaphragmatic Hernia; Boston Children’s Hospital
3. Congenital Diaphragmatic Hernia; Seattle Children’s Hospital
4. Congenital Diaphragmatic Hernia (CDH); C.S Mott Children’s Hospital
5. Congenital Diaphragmatic Hernia (CDH); Cincinnati Children’s Hospital
6. Improving Survival for Infants with Congenital Diaphragmatic Hernia; Johns Hopkins Medicine
7. Congenital diaphragmatic hernia; US National Library of Medicine
8. Diaphragmatic Hernia; Centers for Disease Control and Prevention
Community Experiences
Join the conversation and become a part of our nurturing community! Share your stories, experiences, and insights to connect with fellow parents.
Read full bio of Dr. Pooja Parikh
Read full bio of Dr Bisny T. Joseph
Read full bio of Rohit Garoo
Read full bio of Shinta Liz Sunny