Image: Shutterstock
Candida is a yeast that commonly resides in our bodies, specifically in the skin, digestive tract, birth canal, and oral cavity. While healthy levels of candida may be beneficial, its overgrowth could lead to infections such as breast yeast infections (1).
Yeast infections often occur in warm, moist skin regions such as the underarms, private areas, and skin folds of the breasts and nipples (2). This type of yeast infection affecting the skin is known as cutaneous candidiasis. Fortunately, breast yeast infections can easily be treated and prevented with certain measures. Read on to understand the causes, symptoms, treatments, and management of breast yeast infection and similar skin conditions.
Key Pointers
- Yeast infection of the breasts appears as painful and itchy rashes that are treatable.
- The infection may arise due to excessive sweating, weakened immunity, or poor hygiene.
- Your doctor may carry out a physical examination followed by applying antifungal medications. Nursing mothers are recommended oral administration of lactation-safe drugs.
- Try to maintain proper hygiene, strong immunity, and wear breathable clothing to prevent the infection from developing.
What Are The Signs Of Yeast Infection Of The Breasts?
In healthy individuals, many types of yeasts live on the skin naturally. However, the overgrowth of the yeast Candida can invade the skin surface, causing lesions that can lead to an infection. The lesions of such yeast infection under the skin folds of the breast have the following characteristics (2) (3).
- Bright red patches and rashes
- Redness or pustules around the rash
- One or more patches of different sizes and shapes
- Itching
- Stabbing or shooting pain at the rash
- Radiating burning sensation in one or both the breasts
Additionally, the skin surrounding the lesions may appear dry, cracked, and flaky. Sometimes, the rashes may also produce blisters that ooze fluid (10).
If you notice any of these symptoms, consult a doctor or a lactation consultant to confirm yeast infection and rule out other problems.
 Point to consider
Point to considerOther Skin Conditions With Similar Clinical Appearance
Several skin conditions may present similar symptoms and lesions on breasts as those experienced in a yeast infection. Some of these skin conditions with similar breast rash are (11):
- Eczema: It is a chronic dermatological condition characterized by dry, itchy, and bumpy skin lesions, which may also appear on breasts, specifically in the areolar region.
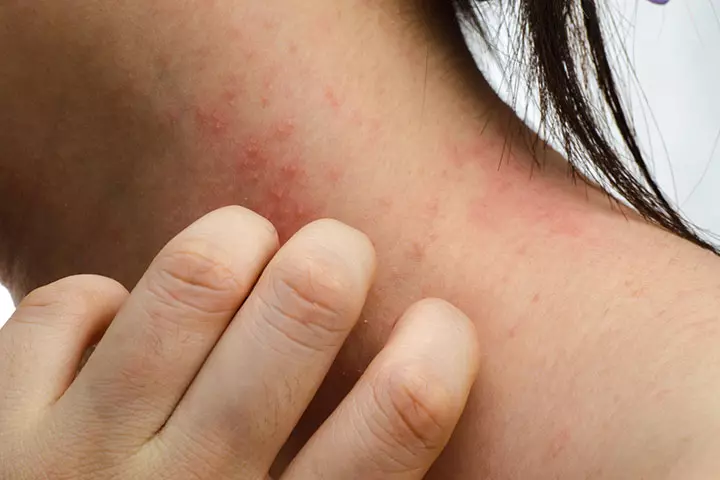
- Allergy: It is an allergic reaction to metals, foods, perfumes, chemicals, fabrics, and other things that may cause a localized rash on the breast.
- Seborrhea: A type of dermatitis, this skin condition usually appears on the scalp characterized by red, dry, flaky, and itchy skin. However, in some cases, it may appear on the breast too.
- Psoriasis: It is a chronic autoimmune skin condition characterized by inflamed, scaly, dry, and itchy patches on the skin, which can appear anywhere on the skin, including the breast.
- Heat rash: This skin condition is characterized by the appearance of a group of tiny, itchy bumps on the skin, including the breasts. It occurs due to blocked sweat glands.
- Cellulitis: It is a bacterial skin infection characterized by red, inflamed, and warm skin rashes along with fever and chills. It can occur on the skin folds of breasts (12).
Dermatologist Dr. Jill Chitalia opines, “The texture of the yeast-infected skin under the breast often feels soggy or overly soft, almost macerated. Conditions like psoriasis or seborrheic dermatitis tend to be drier and scaly. Ruling out these chronic dermatoses is key before starting antifungal therapy.”
A doctor can help you differentiate between these lesions with the help of necessary tools and tests.
Causes And Risk Factors Of Yeast Infection Of The Breasts
Fungal infections, including yeast infections, fundamentally occur when the fungus receives favorable conditions, such as a warm and moist environment, to thrive. Another leading cause is a poor immune response, often due to hampered immunity since the immune system keeps fungal growth in check.
The following are the commonly identified causes and risk factors of a yeast infection on the breasts (2) (3) (4) (5) (6).
- Poor hygiene
- Tight clothing or synthetic clothes
- Ill-fitting shirts and bras
- Infrequent undergarment change
- Excessive sweating due to conditions, such as hyperhidrosis, or hot and humid weather
- Obesity
- History of vaginal yeast infection
- Type 2 diabetes

- Weak immune system
- Existing fungal infections
- Medications, such as steroids, antibiotics, and chemotherapy drugs
- Women with larger breasts may have more skin folds, causing more sweating under the breasts
A doctor diagnoses most cases of breast yeast infections through visual examination or laboratory examination of the nipple discharge. The doctor may scrape a part of the lesion and use the potassium hydroxide (KOH) preparation test to confirm the presence of fungus (7) but it is not always necessary to confirm yeast infection, usually, a physical exam will suffice.
Treatment For Yeast Infection Of The Breasts
The treatment of yeast infection depends on the location and severity of the infection. The treatment includes:
- Topical applications of antifungal drugs, such as powders, creams, and solutions, are most commonly prescribed. Some commonly used topical drugs for fungal infections are Miconazole, Nystatin, Clotrimazole, Oxiconazole, Ketoconazole, Econazole, and Ciclopirox (1) (10).
- Lactating mothers of exclusively breastfed infants may be prescribed lactation-safe oral antifungal medicines, such as fluconazole, to prevent the risk of the baby ingesting the topical medication.
You may take acetaminophen or ibuprofen to deal with breast pain due to the infection (13). - If the infection and rashes do not go away after antifungal medications for a few weeks, doctors may prescribe steroid creams for symptomatic relief (10).
- If you’re a nursing mother, express and store the breast milk to feed your baby before applying a topical medicine on the breasts.
- If fungal infection results from underlying conditions, such as a weak immune system or type 2 diabetes, the doctor may refer you to a relevant specialist.
Correct management of the underlying risk factors accompanied by antifungal medication can cure yeast infection in three to four weeks.
Home Remedies For Yeast Infection
In addition to antifungal medications, some home remedies may also help relieve the symptoms of breast yeast infection and manage the condition. Some of these remedies include (13) (14) (15):
- Use talcum powder to keep the infected area dry.
- Expose the infected area to the air, reducing moisture, which is conducive to the spread of the fungus.
- Apply oregano or coconut oil to reduce nipple irritation.
- Eat yogurt and other probiotics that could help.
- After feeding your baby, rinse the nipples with vinegar and water solution, which is made by adding one tablespoon of vinegar to one cup of water.
Prevention Of Yeast Infection Of The Breasts
Nurse practitioner Shawnda Dorantes says, “One thing I always tell patients: fabric matters. Synthetic bras can trap moisture, so opting for breathable cotton or moisture-wicking materials can make a big difference. Proactively using a gentle antifungal powder in high-risk areas, especially during warmer months, can also help prevent recurrence.” Maintaining good hygiene is the primary way to prevent yeast infection of the breasts. Some other steps that may help prevent the yeast infection include (10) (13) (14):
- Wash your hands frequently
- Wash the skin under your breasts with soapy hot water during a shower
- Give breasts ample time to dry before wearing a bra
- Avoid wearing an ill-fitting bra that restricts airflow

- Give yourself bra-free time at home whenever possible, especially when sleeping
- Change your bra daily and wash them with warm, soapy water
- If you have large breasts, wear supportive bras
- Wear clothes of breathy fabrics, such as cotton and linen
- Avoid wearing very tight clothes
- Do not be in wet or sweaty clothes for too long
- Change your breast pads frequently
- If wearing disposable breast pads, choose ones without waterproof liners. If you’re breastfeeding, change breast pads after every feed
- Try to maintain your body weight in the healthy BMI range
- Maintain your blood sugar levels if you have diabetes
- If you are on any medicines that suppress immunity, such as steroids, ask your doctor if you need preventive antifungal medications
 Quick tip
Quick tipYeast Infection Vs. Thrush
Thrush is also caused by the candida albicans, which is a type of yeast fungi. However, thrush indicates the oral cavity is involved and may cause symptoms such as white patches and inflammation. Yeast infection of the breasts may spread through the nipple to cause oral thrush in babies, especially if a breastfeeding mother is experiencing soreness or cracked nipples. A mother may also develop a candida infection of the breast if her breastfeeding baby has oral thrush.
The condition is also treated with oral or topical antifungals. The same medication that can be used to treat your baby’s thrush (oral nystatin typically) can be used on the breast to provide some relief. The best time to give your infant nystatin is after feeding so it stays in the mouth longer. You usually use a dropper for dispensing the liquid into the infant’s mouth and making sure you place it in the cheeks or areas of white patches. It is usually used four times a day. Talk to your doctor about the dosing and how long to treat.
Frequently Asked Questions
1. Can I pass the yeast infection to my baby through breastfeeding?
Yes. You may pass the yeast infection to your baby through breastfeeding. The baby can also pass the infection to the mother through the mouth (baby thrush). So, this cycle may continue until you receive treatment (5).
2. Do I have to throw out pumped milk if I have thrush?
If your breasts are painful because of the infection, you may give your baby freshly expressed breast milk. However, you should throw away the extra milk and do not store or freeze it for later (8).
Cutaneous candidiasis is the most prevalent cause of breast yeast infections, affecting the skin folds under the breasts and nipples. Although it might have similar symptoms to eczema, skin allergies, and other skin infections, breast yeast infections are readily treatable and preventable if certain precautions are taken. Therefore, contact your doctor for early diagnosis and treatment if you suspect a breast yeast infection. Adequate hygiene, keeping the breast area dry, changing breast pads frequently, and wearing clothes and innerwear made from breathable fabrics can help prevent breast yeast infections.
Infographic: Home Remedies To Get Rid Of Breast Yeast Infection
Severe yeast infection of the breasts requires medical intervention. But you may also try some home remedies to help eliminate its itchiness, rashes, and burning sensation. You will find some simple remedies in the infographic below that you could try to relieve the infection.
Some thing wrong with infographic shortcode. please verify shortcode syntax
My baby and I have had thrush for a month. Should I throw away the breast milk I’ve stored? Find out in this video!
References:
- Candidiasis (Yeast Infection); MSD MANUAL
https://www.msdmanuals.com/en-in/home/skin-disorders/fungal-skin-infections/candidiasis-yeast-infection - Candida infection of the skin; U.S. National Library of Medicine
https://medlineplus.gov/ency/article/000880.htm - Breast & nipple thrush; The Women’s
https://www.thewomens.org.au/health-information/breastfeeding/breastfeeding-problems/breast-and-nipple-thrush - Intertrigo and Secondary Skin Infections; AAFP
https://www.aafp.org/pubs/afp/issues/2014/0401/p569.html - Candidiasis; National Organization for Rare Disorders (NORD)
https://rarediseases.org/gard-rare-disease/systemic-candidiasis/ - Yeast Infection While Breastfeeding; Kaiser Permanente
https://healthy.kaiserpermanente.org/health-wellness/health-encyclopedia/he.thrush.hw139068 - KOH Preparation; PeaceHealth
https://www.peacehealth.org/medical-topics/id/abq2694 - Breastfeeding and thrush; NHS
https://www.nhs.uk/conditions/baby/breastfeeding-and-bottle-feeding/breastfeeding-problems/thrush/ - Nipple Yeast Infection; Cleveland Clinic
https://my.clevelandclinic.org/health/symptoms/22968-nipple-yeast-infection - Yeast Infection Under Breast; Cleveland Clinic
https://my.clevelandclinic.org/health/diseases/22970-yeast-infection-under-breast - Breast Rash; Cleveland Clinic
https://my.clevelandclinic.org/health/symptoms/17885-breast-rash - Skin-associated Infection (Cellulitis); Breastcancer.org
https://www.breastcancer.org/benign-breast-conditions/cellulitis - Candida or thrush of the nipple and breast Patient handout; Jewish General Hospital
https://cdn.ciussscentreouest.ca/documents/hgj/pfrc/Breastfeeding_clinic/Thrush_px_handout_2019.pdf - Jenny Bowen; Yeast Infection Care while Breastfeeding; Corporate Lactation Services
https://corporatelactation.com/wp-content/uploads/2026/08/CORNING-Info-On-Yeast-Infections-Handout-2.pdf.pdf - Breastfeeding challenges; NHS
https://www.nhs.uk/start-for-life/baby/feeding-your-baby/breastfeeding/breastfeeding-challenges/thrush/
Community Experiences
Join the conversation and become a part of our nurturing community! Share your stories, experiences, and insights to connect with fellow parents.
Read full bio of Dr. Ashley Van Putten
Read full bio of Dr. Ritika Shah
Read full bio of Swati Patwal
Read full bio of Ghazia Shah